My name is Jessica, and I am a wife, a mom to two beautiful children and a permanent ileostomate.
A difficult pregnancy
I was diagnosed with Crohn’s disease in 2007, 10 months after the birth of my first child. My pregnancy had been less than stellar, as it involved what I now know was my first official Crohn’s flare. Throughout my pregnancy, I experienced uncontrollable diarrhoea and an overall feeling of not being well. My daughter was born prematurely, at 32 weeks and 5 days, and she spent 12 days in the neonatal intensive care unit.
Just 2 weeks after my daughter’s birth, I was at my pre-pregnancy weight—a mom’s dream, right? Still, I was having new troubles, with uncontrollable bathroom runs, major pain when peeing and constant burning in all areas down below.

Jessica strong and healthy at 41
Worsening diagnoses
After a visit to primary care, I was diagnosed with a urinary tract infection and put on a course of antibiotics. From there, things went terribly downhill. On the evening of 3 January 2007, I was rushed to the emergency department by my mother-in-law, while my husband remained behind with our now 6-week-old. At this point, I was having nightly sweats and fevers, and I couldn’t control my bowels or even sip water. When my mother-in-law arrived, I was in the foetal position, crying and hallucinating.
I was admitted to hospital for 7 days, and, upon discharge, I was sent home with a possible diagnosis of Crohn’s disease or a bacterial infection (Clostridioides difficile) and a referral to follow up with one of the hospital’s gastroenterologists. After a few months, my husband and I decided to switch and seek a second opinion from a different gastroenterologist, based at a university hospital. In September 2007, just shy of my 29th birthday, I was diagnosed with indeterminate Crohn’s colitis. I had a very diseased large intestine, with patterns of striations, deep-lining inflammation and ulcerations from the ascending colon to the anus.
Eating and drinking with an ileostomy
When it comes to food, I prefer to eat smaller-portioned meals, to eat slowly and to chew, chew and chew. I learned that fruit and vegetables affected my stoma’s output, but I was happy to realise that I didn’t have to eliminate these foods, I just had to prepare them differently to how I was used to.
People with an ileostomy are at risk of dehydration and so need to keep well hydrated and topped up on electrolytes (salts). I drink plain, flat water with all my meals, and I start every single day with 220 ml of warm water, a few pinches of pink Himalayan salt and a quarter of a freshly squeezed lemon.
You can often gauge whether you need more electrolytes according to the colour of your pee. Before relying on special electrolyte drinks, I recommend first drinking plenty of water and eating a varied wholefood diet with lots of salt. However, it may be worth having an electrolyte drink on hand for hot, sweaty and intense workouts.
Living with disease
I battled the disease for the next 3 years. I tried a variety of different medications and combinations of medications and alternative therapies. We even sought the opinion of three more gastroenterologists, hoping that they’d spot something that the others didn’t.
We heard that, in the world of American gastroenterology, the best of the best were based in and around North Carolina. In February 2010, my husband and I made the bold decision to move there, from Massachusetts, even though we had no family, friends or support network in the area. By August, we found a rental and made the drive, with our now 3-year-old daughter.
In North Carolina, I met with two more gastroenterologists, and I also had weekly sessions with a psychologist who specialised in working with people with chronic illnesses. In March 2011, after exhausting all medication options available at the time, I met with a gastrointestinal surgeon, Dr Sadiq, and the most awesome wound, ostomy and continence nurse (WOCN), Lara, with whom I am still friends almost 11 years later. I was so sick that I asked for them to schedule the surgery that day, despite not knowing what a stoma or ileostomy was.

The Ormondroyds at Christmas 2020
Information and support
I had to wait 4 weeks for my surgery. Dr Sadiq sent me home with some literature, along with instructions not to Google things. Let’s say that I was concerned, and I wanted to learn as much as I could. Once I had read through all the materials I’d been given, what did I do? Of course, I went to Google to do my own research. It turned out that Google can be helpful as well as, and I found forums where people with an ostomy can share stories and advice, as well as the United Ostomy Associations of America (UOAA).
With 2 weeks to go before my surgery, I attended my first local ostomy group, affiliated with the UOAA. There was a bunch of new people at this meeting, and I was happy to meet four other young women there. I sat and listened to the speaker, and, when the event was opened to questions, I was able to ask about people’s experiences of surgery.
I felt so terrible that, honestly, I wasn’t scared of having surgery. It wasn’t until the wee hours of the morning, an hour before I had to leave for the hospital, that I broke down in tears to my mom. She had travelled 800 miles to help care for our now 4-year-old daughter.

Jessica and family 8 weeks post-op
Surgery
There was nothing textbook about my disease, and there was nothing textbook about my surgery or hospital stay. It all took longer than expected, and there were complications. I remember how emotional I was when I awoke and saw my stoma for the first time and had to do my first pouch change. As tears streamed down my face and my family watched, I will never forget Lara’s words: ‘I know this is hard and new, but I promise that you will be okay and feel so much better’, before she gave me a hug.
During my hospital stay, I was lonely. Thankfully, Christie, an ostomate from a support group, worked in the hospital, and she came to visit me and brought me a bag of goods that would make my hospital stay a little more doable. I was in a faraway land, away from most of my family and long-time friends. But, with the support of my husband, mom, stepdad and in-laws, I survived every complication, blockage, catheter, nasogastric tube, prick and prod during my 21-day hospital stay.
Jessica’s top tips for getting fit after stoma surgery
• Discuss your exercise goals with your team during postoperative follow-up and only start working out when they give you approval (typically 6–8 weeks postop)
• Remember that there is no need to rush into things, and start small, with daily walks as soon as you feel up to it
• Put safety first and practice good form and technique
• If your stoma hurts during a workout, stop what you are doing and evaluate what might be causing the discomfort
• Prioritise learning how to engage your core strength, which is important for reducing the risk of complications, but something that few people know how to do properly
• Find the right pouching system that will give you a long wear time and is unlikely to sweat off or leak
• Make an informed decision about whether to wear an ostomy support garment (belt or underwear)—personally, I am a fan of high-waisted shorts and leggings!
New life
From there, my quality of life was dramatically different. After 8 weeks, I was able to go on a cruise; at 18 weeks, I started back at the gym; and soon I was finally able to be the wife and mom I had so longed to be.
My wounds took almost a year to heal. I had allergic reactions to different products, but I figured it out. I didn’t get discouraged, because I had been through a hell of a lot more. Of course, there were tiny blips in the journey, but they only made me stronger.

Jessica and husband on horseback at Punta Cana in the Dominican Republic, April 2017
Little man
In March 2012, 11 months post-op, we found out I was pregnant again. It was one of the happiest, and one of the scariest, times of my life. I couldn’t find anyone else with an ileostomy who was pregnant to talk to. Again, it was one of those things where I had to figure it out on my own.
My pregnancy went pretty seamlessly. I was given weekly progesterone shots, since I had a history of preterm labour. I worked out at the gym 5 days a week, doing weights, cardio and Zumba. There was nothing more therapeutic than busting a move with a big old belly. My little man loved to bust a move with me, although he did seem to hate it if the music was too loud.
At 30 weeks, my ob-gyn had me stop exercising for fear of preterm labour, and at week 31 we were stopping progesterone. Sure enough, a few days after, when I would normally get my shot at 32 weeks, I started preterm labour. Thankfully, the medical team stopped the labour and put me on full bed rest. Little man stayed put for 3 more weeks and was born vaginally.
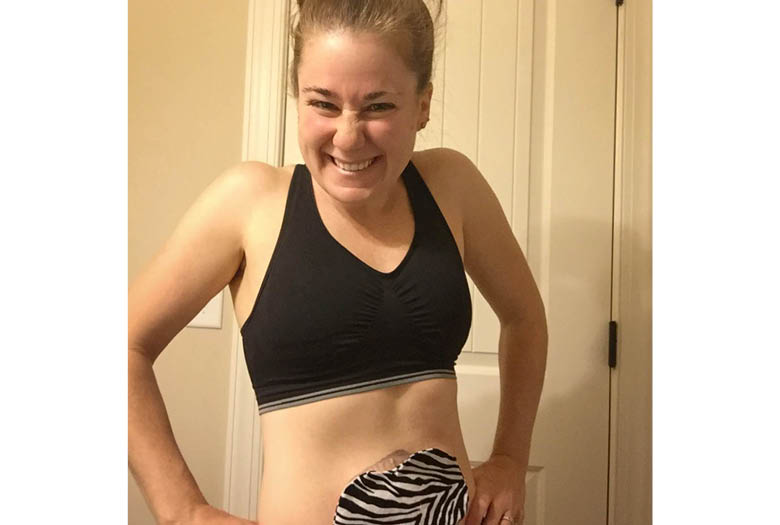
Jessica and her ileostomy
Overindulgence
Over the next 3 years, I was in a constant struggle with weight gain and weight loss. This was because I was in remission, and so—let’s be real—I could finally eat! I was overindulging in the foods that I love, but these weren’t what could be called healthy options. I also think that I was allowing myself to eat to relieve the stresses that came with being a new mom again, having kids 6 years apart and taking care of a youngest child who had been diagnosed with a tongue, throat and swallowing disorder.
I continued to work out at the gym and volunteer as much as I could at my daughter’s school. While I was generally healthy, I still felt a bit lost. I had mom friends, now including the moms of my son’s preschool friends, but I still felt like I was missing something. I was home with both kids, while my husband travelled for work each week, and the rest of my family were far away.
Jessica’s top tips for living well with a stoma
• Be patient in learning about your ostomy, what works and what doesn’t, as it’s a process and journey that takes time
• Try not to compare your journey to anyone else’s, as no two ostomies are the same
• Practice self-care in a way that is right for you
• Seek professional help when it is needed
• Look for the solutions that allow you to do the activities you love without being limited by your ostomy
Back to my roots
Back in Massachusetts, from 2001 to 2010, I had been a special education teacher, and I wanted to go back to my teaching roots. I had always played sports, and I played Division I collegiate field hockey, so I was no stranger to working out. So, in 2015, I decided to become a health and fitness coach.
I started working on myself first, by getting back to a routine of healthy eating, regular exercise and personal development. I confronted my habit of overeating as a coping mechanism and found healthier ways to cope. Now, I am able to help women and men all over the world, providing them with the tools and resources to lead their healthiest lives, whatever that means for them.
Believe in yourself
One of the hardest things about what I do is believing in everyone more than they believe in themselves. I try to show the people I work with that we are capable of so much more than we think we are. Likewise, I hope that everyone reading this will recognise how brave and strong they are and remember that they are never truly alone.
Jessica Ormondroyd is a health and fitness coach and lives with her family in North Carolina, USA


