Becoming pregnant with a stoma can feel like an absolute blessing. In some cases, abdominal illness and surgery can make conceiving a child difficult or impossible, and this can be on the minds of many people, especially women, going for stoma-forming surgery.
My experience
I have inflammatory bowel disease (IBD), which led to me undergoing a proctectomy (‘Barbie butt’ surgery) and getting a stoma. Flare‑ups of IBD have caused me to have numerous miscarriages in the past. I was told I wouldn’t be able to have children, and, after trying for a while, my partner and I decided to give up. I resigned myself to feeling that it was never going to happen.
So, when I most recently found that I was pregnant, I had no idea what to expect. I was just 6 weeks pregnant when I had the first positive pregnancy test. So many thoughts ran through my mind. Initially, I certainly worried whether my stoma would be okay, especially I had heard that it is easier to get a hernia or a prolapse during pregnancy, but my main worry was that I would miscarry again.
However, at the time of writing, I have been pregnant for 29 weeks, and I would like to share my experiences and advice.
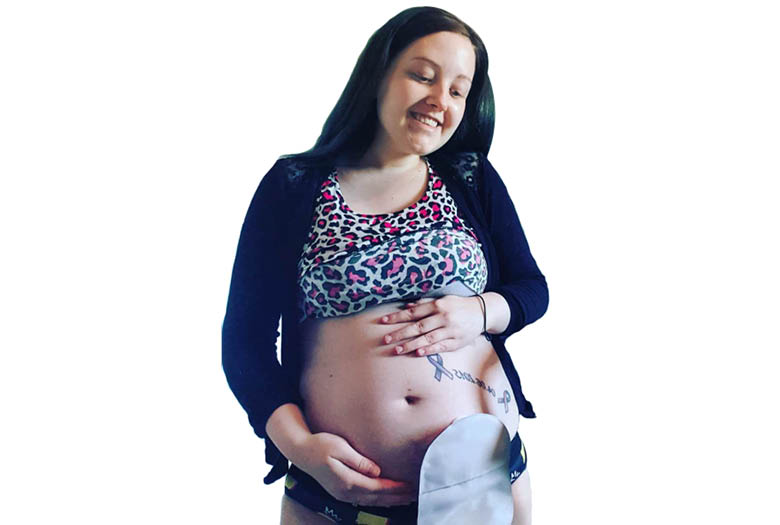
Pregnancies are all very different
Early stages
In my local health service, if you suspect that you are pregnant, the first thing to do is arrange an appointment with your GP for a pregnancy test. This might be accompanied by some blood tests. It the test comes back positive, the GP will give you the contact details for a local midwife, who you can call to arrange an appointment with.
I became pregnant during the COVID-19 pandemic, and so my first midwife appointment was over videocall. This was a welcome relief, as, at the time, I was vomiting a lot, and I was dreading the thought of getting up the energy to travel anywhere (or even have a shower). Once you are in touch with the midwife, it becomes a waiting game. At 12 weeks, you have a scan and meet the pregnancy team who will take care of you and the baby. At this discussion, the team will answer questions, offer advice and jointly decide whether your pregnancy and delivery plans should be led by a midwife or a consultant. Depending on your medical history, the pregnancy team may also get in touch with your surgeon or IBD team for their input.
Eating and drinking for two
There are a few tips for what you eat and drink that can be very beneficial during pregnancy:
-
- It’s important, especially if you have an ileostomy, to avoid dehydration, which you can do by keeping on top of your electrolytes with special drinks
- If you find you get constipation, it is worth adjusting your diet to avoid anything too heavy and have more liquid foods, such as soups, as well as drinking orange juice
- In general, it’s better to eat smaller meal portions throughout the day, rather than big heavy meals
- When pregnant, always keep some snacks nearby—you will thank me later!
Changing times
Some people’s stomas stay the same as ever throughout their pregnancy, while others go through some changes.
During my pregnancy, my stoma changed a lot. The main change that I noticed was the size of my stoma, which grew from its normal 25–30 mm to a much bigger 40 mm. This made it harder to pass output and caused some regular uncomfortable constipation. Then, as my baby bump grew bigger, it started to put more pressure on the skin around my stoma (peristomal skin), which made things like coughing or blowing my nose also rather uncomfortable. To top this off, my bowel became less tolerant of foods that it had previously been okay with. This caused some blockages, which required a couple of trips to the hospital at silly times in the morning to resolve. If you find that you are having fewer bowel movements, feeling unusual pain and/or generally feeling unwell, you should contact your GP or an out-of-hours service straight away.
It has not all been so tough, and I have found that emptying my pouch with my bump has been super easy.
A few of my friends are ostomates who have had children or are pregnant. When I have spoken to them about this, many say that they had no issues at all with their stoma during pregnancy, while a few others had some issues with their stoma swelling at times. So, it seems that pregnancies are all very different, and everyone has their own individual experience.
If you do struggle with your stoma at all, or if you have any stoma-related questions, please contact your stoma care nurse as soon as possible.
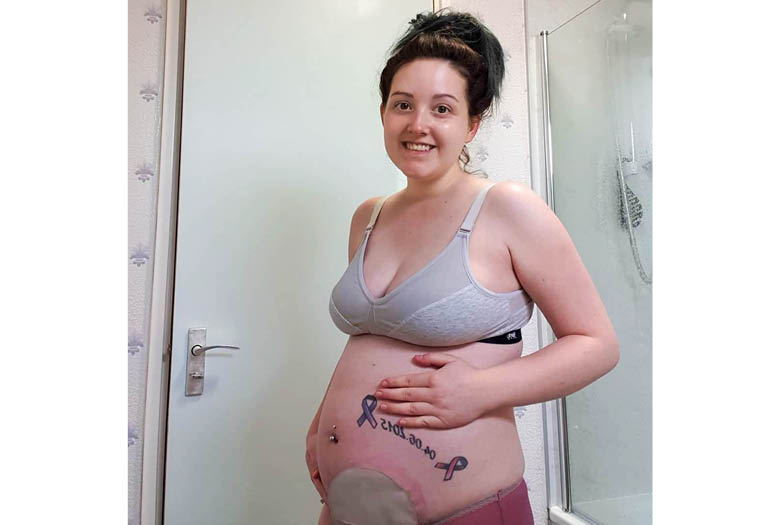
Being pregnant is rarely easy
Making progress
Your experience will likely change as your pregnancy progresses. From around 16 weeks, you will feel butterflies in your stomach as the growing baby starts to move. This can feel very strange to start with. Soon, by around 20 weeks, you should experience some kicking.
It is important to know that, if you get reduced movements or none at all, you should call the emergency number given to you by your midwife. I was advised to try drinking a sugary drink to encourage the baby to move, and, in my case, it certainly seemed to work.
Your pregnancy can also be affected by your environment. I’ve been pregnant throughout the summer, and dealing with the heat has been particularly hard. A fan and nighties have been absolute essentials.
Having offered all these tips, I should also say that pregnant people often receive a lot of well-meaning but unwanted advice from others. If this happens to you, I encourage you to feel that you can speak up from the get-go. You have the right to let people know, politely but firmly, that you don’t want their advice.
Look after number one
By all means, being pregnant is rarely easy. In reality, there are parts of pregnancy that are not so great, and these are rarely spoken about. If you find yourself having bad days or a not-so-great pregnancy in general, it’s good to remember that you are not alone, and you needn’t feel bad about it.
When good days do come, you can make the most of enjoying them. This might just mean resting when you need to rest, especially during the first trimester, when you may find yourself sleeping and napping more than normal. What is important is to look after yourself.
Alannah Jayne Simpson lives in Aberdeenshire, Scotland, and runs a blog with Trio Ostomy Care